mmWave Radar for Contactless Monitoring of Heart and Breath Rates
Vital signs—body temperature, blood pressure, breath rate, and heart rate—offer clinicians immediate insight into a patient’s health status and the trajectory of recovery or decline. These metrics vary with age, gender, weight, fitness, and current physical or mental activity. For example, during exercise, body temperature, breath rate, and heart rate naturally rise.
Millimeter‑wave (mmWave) radars transmit short‑wavelength radio waves that reflect off objects, allowing the system to deduce range, velocity, and angle with millimeter‑level precision. This capability makes mmWave an ideal, contact‑free platform for continuous vital‑sign monitoring, eliminating the need for adhesive sensors and reducing infection risk—particularly important during pandemics.
In this article we explore how mmWave radar can detect breath rate (BR) and heart rate (HR), the challenges involved, and the emerging healthcare applications.
What Do BR and HR Reveal?
Typical healthy ranges for BR and HR are summarized below (Table 1). Individual values differ by age, gender, fitness, and activity level, so a combined assessment of HR and BR helps clinicians gauge stress and overall well‑being.
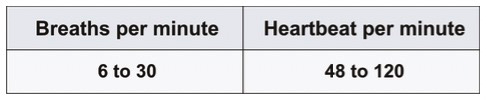

Table 1: Vitals of a Healthy Person
Age‑specific resting heart rates are detailed in Table 2 (source: Wikipedia).
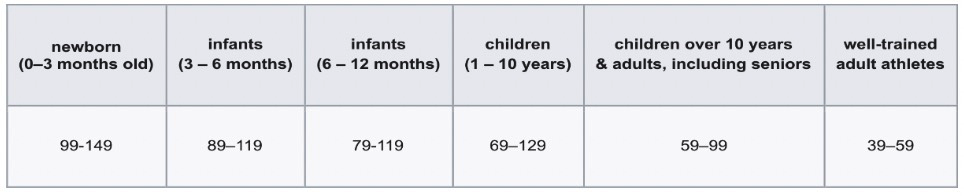

Table 2: Age‑wise Resting Heart Rate
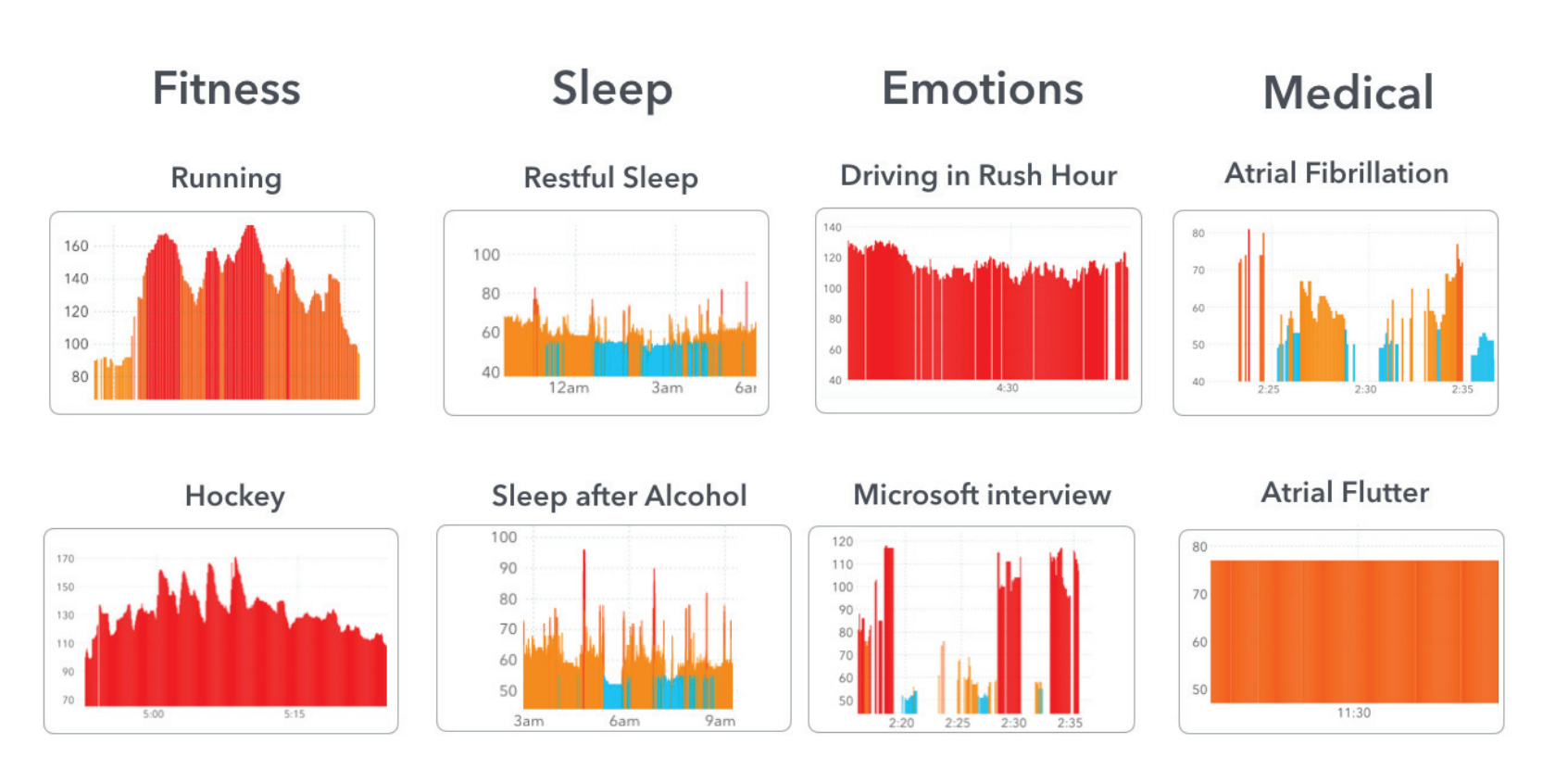
Figure 1 illustrates how HR fluctuates with fitness, stress, and medical conditions (source: AAAI 2018).
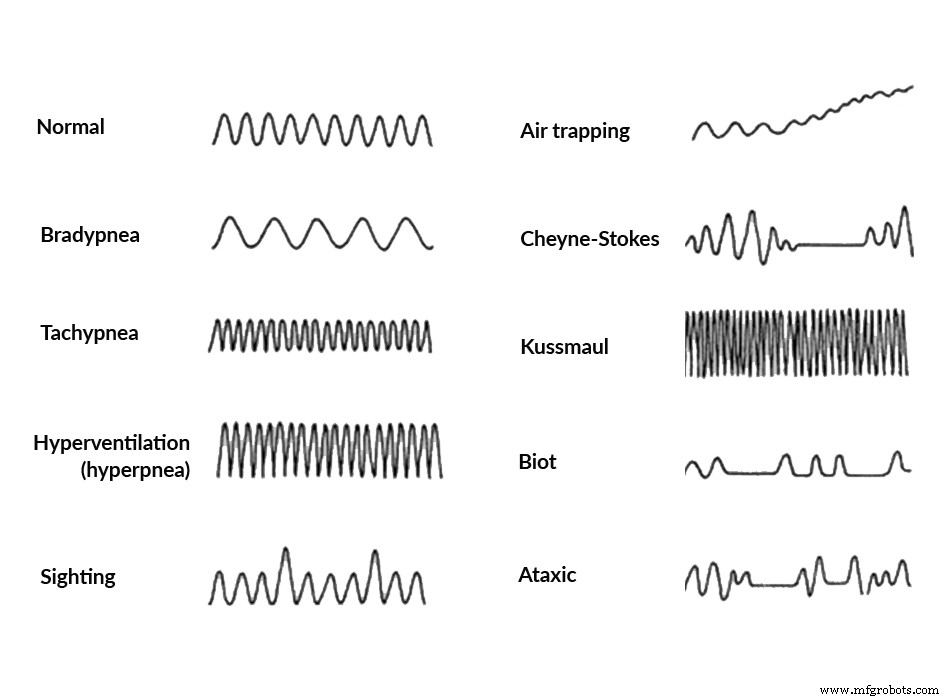
Abnormal BR and HR can signal life‑threatening conditions such as obstructive sleep apnea (OSA), sudden infant death syndrome (SIDS), dyspnea, and chronic obstructive pulmonary disease. Figure 2 shows characteristic breath patterns across these disorders (source: ClinicalGate).
High resting HR correlates with increased cardiovascular risk, while low resting HR may predict future pacemaker need. Continuous, non‑contact monitoring of BR and HR can thus be life‑saving for vulnerable patients.
Contact vs. Contact‑Free Monitoring
Traditional vital‑sign devices—such as ECG electrodes and pulse oximeters—require direct skin contact. For long‑term monitoring, this is inconvenient and increases cross‑contamination risk. Contact‑free sensors, especially mmWave radar, provide a safer alternative by measuring minute chest movements from a distance.
mmWave Radar Fundamentals
mmWave radars operate at 30–300 GHz, corresponding to wavelengths of 10–1 mm. Industrial allocations span 60–64 GHz, while automotive systems use 76–81 GHz. The short wavelength enables compact antennas and sub‑millimeter precision in range detection.
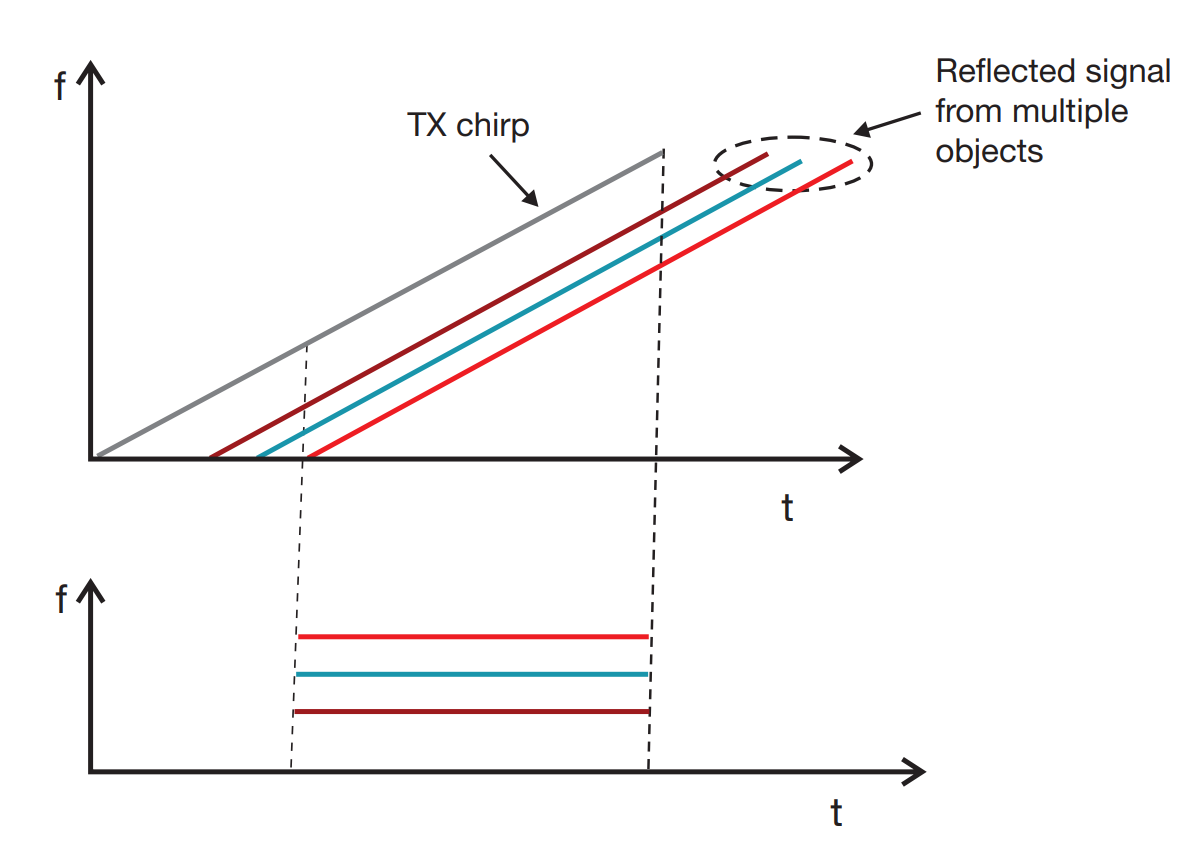
We focus on frequency‑modulated continuous‑wave (FMCW) radars. FMCW transmits a linear chirp—frequency increasing over time—and captures the reflected signal. The difference between transmitted and received frequencies yields distance; phase shifts reveal motion.
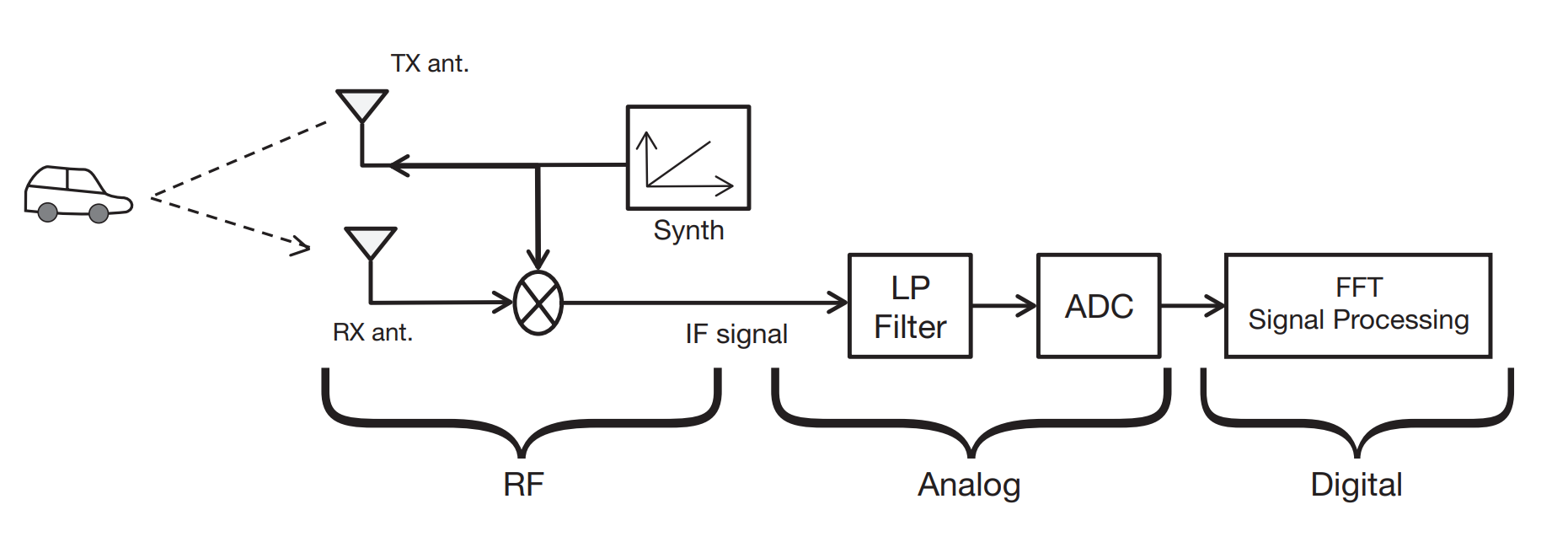
A typical FMCW radar block diagram is shown in Figure 4 (source: TI.com).
The mixer combines transmitted and received signals, producing an intermediate frequency (IF) that contains sum and difference components. A low‑pass filter isolates the difference component, which is then Fourier‑transformed to reveal peaks corresponding to object ranges.
Velocity is derived from phase differences between successive chirps, leveraging the Doppler effect. The short mmWave wavelength (≈ 3.5 mm) amplifies phase sensitivity, enabling detection of sub‑millimeter motions.
Detecting Heart and Breath Rates with mmWave
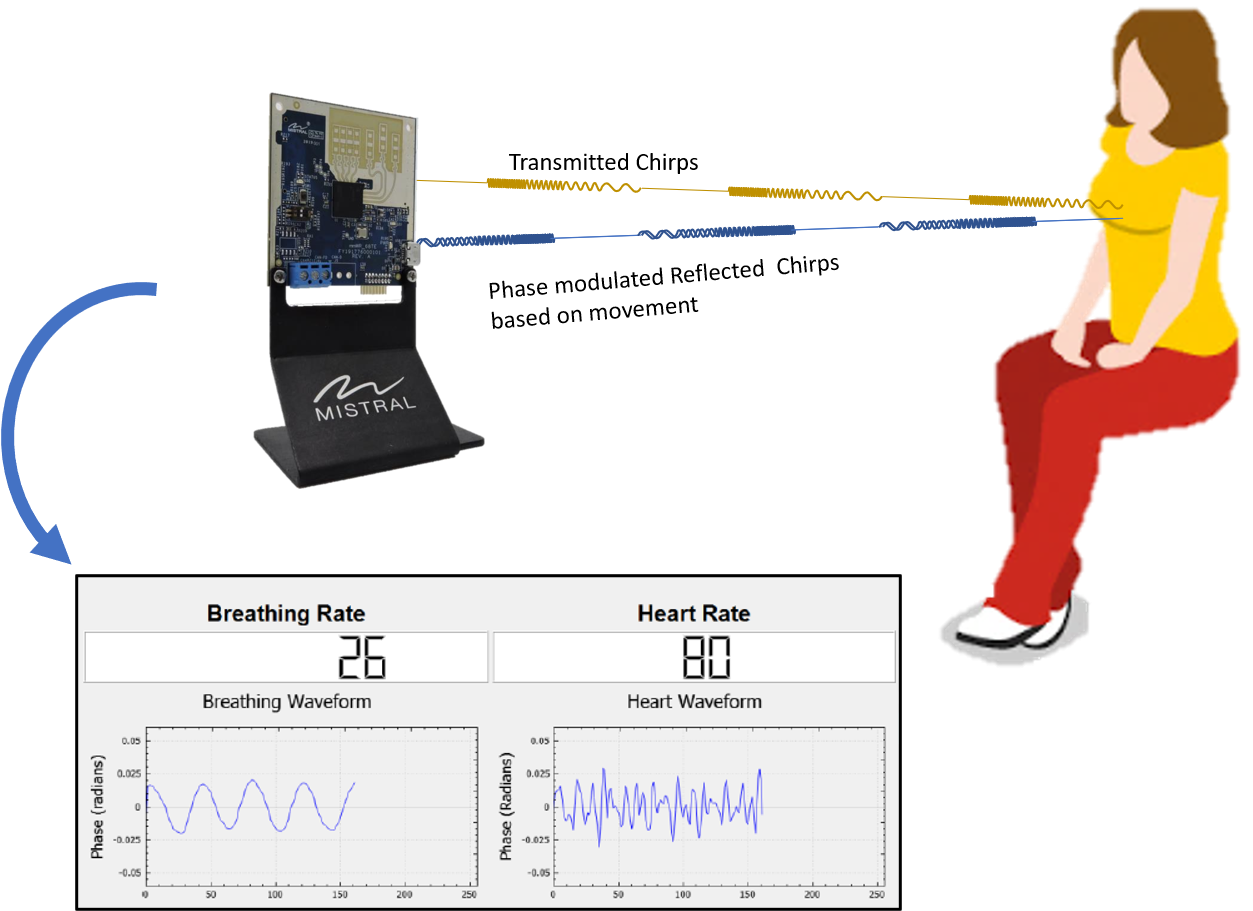
mmWave radars operating at 60 or 77 GHz can sense chest movements as small as a fraction of a millimeter. Figure 6 depicts the signal flow: chirps are transmitted toward the chest, the reflected signal is range‑FFT‑processed to isolate the chest bin, and the phase of that bin is tracked over time.
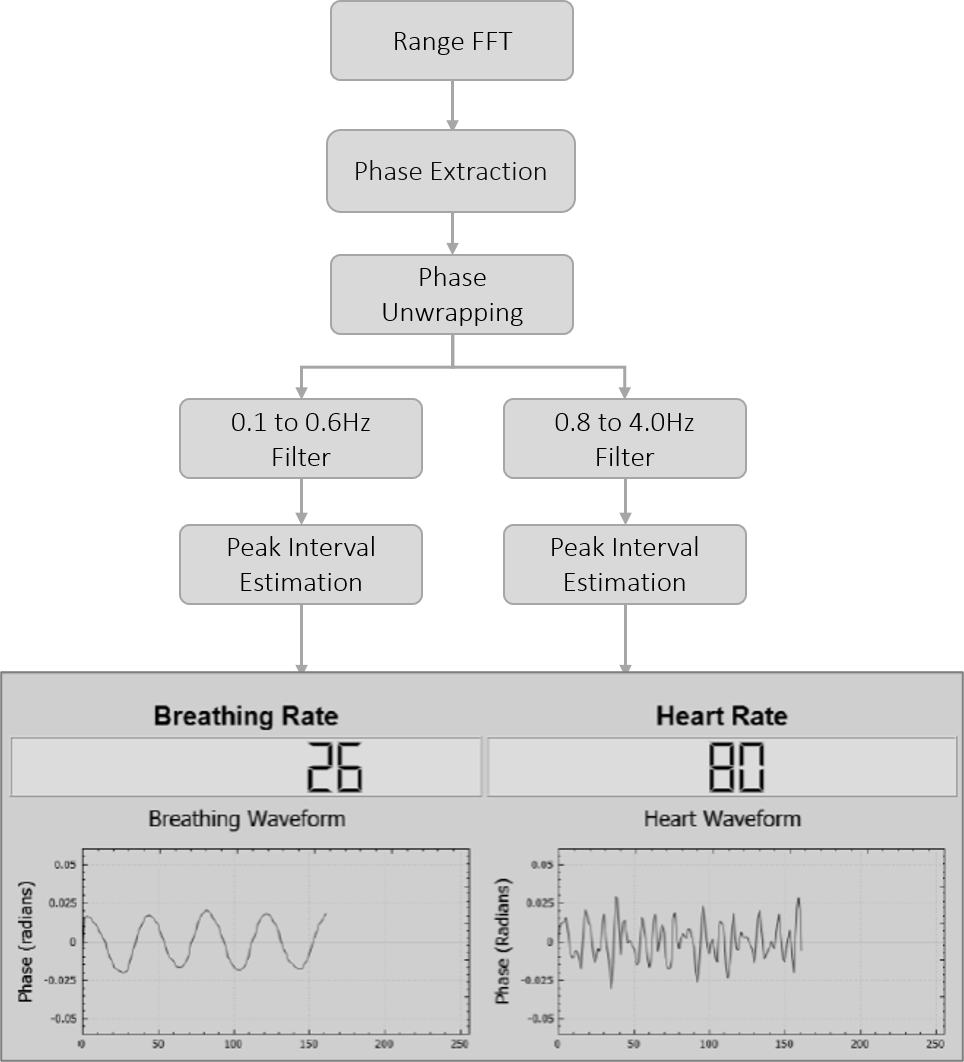
From the velocity time series, a Doppler FFT isolates frequency components corresponding to heartbeats (≈ 0.8–2 Hz) and breathing (≈ 0.1–0.5 Hz). Counting peaks in each one‑minute window yields HR and BR values. Figure 7 illustrates this algorithm.
Challenges and Future Directions
Signal reflection varies across individuals due to differences in skin type, tissue composition, and body water content. Ongoing research into these variabilities aims to refine calibration models and enhance measurement accuracy.
Conclusion
While mmWave radar has traditionally served defense, automotive, and industrial sectors, its evolving precision, rapid signal processing, and ultra‑compact form factor now unlock transformative healthcare applications—patient activity monitoring, vital‑sign surveillance, and even stress or drowsiness detection. These capabilities hold promise not only for clinical settings but also for intelligent driver‑monitoring systems.
References
- Texas Instruments. "68xx Vital Signs."
- "Remote Monitoring of Human Vital Signs Using mm‑Wave FMCW Radar."
- DeepHeart: Semi‑Supervised Sequence Learning for Cardiovascular Risk Prediction.
Sensor
- RFID‑Based Home Security: Low‑Cost, Battery‑Free Monitoring Solutions
- Revolutionizing Health Monitoring: Sensor‑Based Vital Sign Measurements
- Remote Weather Monitoring with Raspberry Pi 3 and PubNub
- Integrated Heart‑Rate Sensors in Smart Clothing: Reliable Wearable Monitoring
- Unified COVID-19 Test: Detect, Track Variants & Co-Infections in One Procedure
- Sensor‑Woven Shirts Offer Real‑Time Vital Sign Monitoring
- Advanced High‑Altitude UAV for Precise Meteorological Monitoring
- Radar-Enabled, Touch-Free Heart Sound Monitoring
- Neural Networks Accelerate X‑Ray Imaging Reconstruction
- Advanced Biosensor Enables Real‑Time Oxygen Monitoring in Organs‑On‑a‑Chip