Gradient Nanomechanical Properties of Fluorosed Enamel: Implications for Restorative Material Selection
Abstract
This study examines the gradient nanomechanical behavior of enamel affected by dental fluorosis and establishes evidence‑based criteria for selecting restorative materials. Nanoindentation (2000 μN load, 30 s hold) and nanoscratch (1000 μN load) tests were performed on the outer, middle, and inner layers of normal enamel, mild fluorosis enamel, and severe fluorosis enamel. The outer layer of mild fluorosis enamel was compared with four restorative materials: lithium disilicate glass‑ceramic (IPS e.max CAD), polymer‑infiltrated ceramic network (PICN), composite resin block (Lava™ ultimate), and conventional composite resin (Fltek™ Z350XT). Results revealed distinct gradient trends: mild fluorosis enamel showed increased nanohardness and elastic modulus from outer to middle layers, then a decline toward the inner layer; severe fluorosis enamel displayed a monotonic increase in hardness and modulus toward the inner layer, with a corresponding decrease in creep displacement. Nanotribological metrics mirrored these trends. The scratch depth and width of Lava™ ultimate matched the outer layer of mild fluorosis enamel, whereas IPS e.max CAD exhibited the lowest scratch depth/width. These findings underscore that fluorosed enamel’s mechanical profile differs markedly from healthy enamel, necessitating restoration materials with compatible wear resistance to avoid excessive abrasion of either the restorative or opposing enamel. (Trial registration: WCHSIRB‑D‑2014‑126, registered 25 December 2014).
Introduction
Dental fluorosis arises when excessive fluoride intake during tooth development alters enamel mineralization [1, 2]. In high‑fluoride regions, prevalence can reach 80–90% [3, 4]. The resulting chalky, opaque patches or structural defects compromise esthetics and function, often leading to psychosocial distress [5]. Restorative intervention is therefore common [6, 7]. Successful restoration depends on matching the mechanical and tribological properties of the restorative material to the opposing enamel to prevent accelerated wear of either substrate [8, 9]. Misalignment can cause rapid degradation of the restoration or the natural tooth [10, 11]. Consequently, a comprehensive understanding of the microstructure, nanomechanical, and nanotribological characteristics of fluorosed enamel is essential for informed material selection [12].
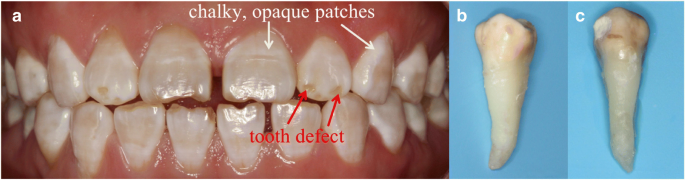
Photographs of dental fluorosis. a Intraoral image of mild fluorosis showing chalky, opaque patches and severe fluorosis displaying both chalky patches and tooth defects. b Extracted mild fluorosis enamel. c Extracted severe fluorosis enamel.
The enamel’s outer layer protects dentin and pulp and must withstand mastication forces over millions of cycles [13, 14, 15]. Its superior mechanical properties dissipate stress and prevent crack initiation [12]. Enamel exhibits a gradient from the outer surface to the enamel‑dentin junction (EDJ), reflecting progressive changes in microstructure and composition [15, 16, 17, 18]. Chronic fluoride exposure disrupts this gradient, causing structural alterations and mechanical property changes [19, 20, 21, 22, 23, 24]. Prior animal studies [22, 23] and a recent human study on mild fluorosis [24] have not addressed the full gradient. This investigation fills that gap and evaluates four restorative materials against the outer enamel layer of fluorosed teeth to guide clinical decision‑making.
Materials and Methods
A total of 30 caries‑free premolars (10 normal, 10 mild fluorosis, 10 severe fluorosis) were extracted from 19‑25‑year‑old donors residing in high‑fluoride areas. The protocol received approval from the West China Hospital Ethics Committee. Teeth were stored in Hank’s balanced salt solution (HBSS, Solarbio, Beijing) at 4 °C to preserve hydration and were tested within one week of extraction.
Sample Preparation
Crown sections were produced using a Struers Minitom with a diamond cutoff wheel (300 rpm, water irrigation). Each crown was split into two halves and embedded in epoxy resin (EpoFix, Struers). One half underwent nanoindentation; the other half was reserved for nanoscratch testing. For restorative materials—IPS e.max CAD, PICN, Lava™ ultimate, and Fltek™ Z350XT—five specimens (4 mm × 4 mm × 2 mm) were polished sequentially from #800 to #4000 SiC paper, then with 3 μm and 0.04 μm abrasive solutions (OP‑S NonDry, Struers), and finally ultrasonically cleaned. Enamel layers were defined as: outer (≤100 μm from occlusal surface), middle (mid‑distance to EDJ), and inner (≤100 μm from EDJ) [25].
Nanoindentation Tests
Indentations were conducted with a Triboindenter TI950 (Hysitron) using a Berkovich diamond tip (~150 nm radius). An integrated scanning probe microscope identified target regions. Load: 2000 μN, holding time: 30 s, loading/unloading rate: 400 μN/s. Fifty indents per enamel layer ensured statistical robustness, with inter‑indent spacing >5 μm. Reduced elastic modulus and nanohardness were extracted via the Oliver–Pharr method [26, 27]. Contact displacements before and after the hold period were recorded, and the difference (changed displacement) quantified creep behavior.
Nanoscratch Tests
Nanoscratch experiments employed the Triboindenter TI950 with a conical diamond tip (~1 μm radius). Scratches were applied under 1000 μN at 0.5 μm/s over 10 μm. Fifty scratches per enamel layer and material were executed, spaced >5 μm apart. The system recorded friction coefficient, scratch depth, and width.
Statistical Analysis
Data were analyzed with SPSS 18.0. One‑way ANOVA and Student’s t‑tests evaluated group differences; p < 0.05 indicated significance.
SEM Observation
Field‑emission gun SEM (INSPECT F, Czech Republic) examined microstructures of all enamel layers.
Results and Discussion
Microstructure and Gradient Nanomechanical Behavior of Dental Fluorosis Enamel
Figure 2 shows SEM micrographs of the three enamel layers for each tooth type. Normal enamel rods were uniform and upright in the outer and middle layers, while the inner layer exhibited an undulating pattern. Mild fluorosis enamel displayed a few pores in the outer layer; the middle and inner layers remained comparable to normal enamel. Severe fluorosis enamel’s outer rods had broadened inter‑rod gaps and numerous pores, with loosely arranged crystals and increased microporosity. The inner layer of severe fluorosis resembled normal enamel. These morphological differences stem from (1) excessive fluoride disrupting enamel matrix protein retention and causing rod hypomineralization [28–31] and (2) chemical substitution of hydroxyl by fluoride in hydroxyapatite, forming fluorapatite [31].
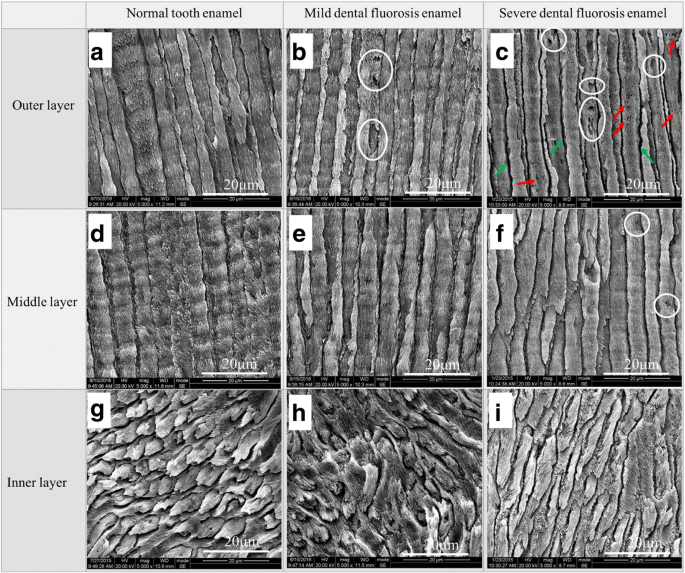
SEM images of normal tooth enamel (a–c), mild fluorosis enamel (d–f), and severe fluorosis enamel (g–i). Layers were etched with 37% phosphoric acid (30 s) and imaged at ×5000. Green arrows indicate broadened gaps; white circles, pores; red arrows, loosely arranged crystals.
In normal enamel, nanohardness and elastic modulus decreased from outer to inner layers (Fig. 3), while creep displacement increased (Fig. 4). This gradient reflects the transition from densely packed rods to protein‑rich inter‑rod enamel and the associated mechanical attenuation [32–34]. In mild fluorosis enamel, hardness and modulus increased from outer to middle layers, then declined toward the inner layer (Fig. 3). The outer layer exhibited a significantly higher creep displacement (7.70 ± 2.71 nm) than normal enamel (p < 0.05). In severe fluorosis enamel, both hardness and modulus rose steadily from outer to inner layers, with the inner layer achieving the highest values (nanohardness 2.04 ± 0.89 GPa; modulus 46.63 ± 11.19 GPa). Creep displacement decreased from outer to inner layers, with the outer layer showing the largest displacement (11.50 ± 3.77 nm) (Fig. 4). These distinct trends underscore the altered load‑bearing capacity of fluorosed enamel.
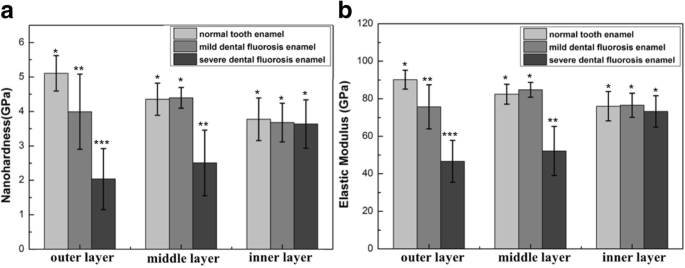
Nanomechanical properties of enamel layers. a Nanohardness; b Elastic modulus. Identical symbols denote no significant difference among corresponding layers across groups.
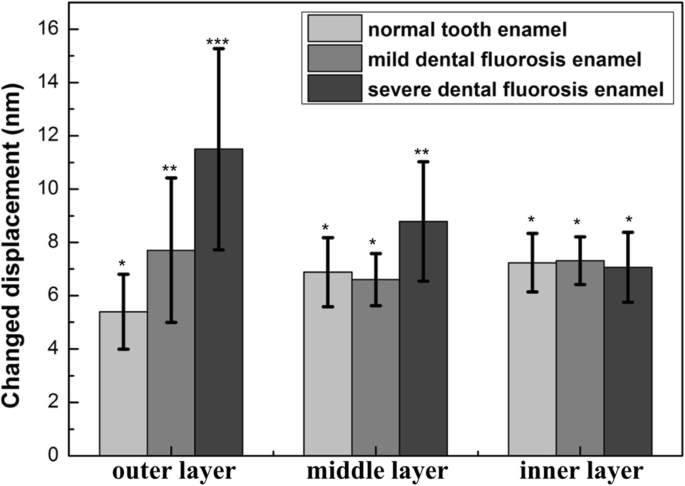
Creep behavior of enamel layers. Identical symbols denote no significant difference among corresponding layers.
Friction coefficients increased from outer to inner layers in normal enamel. In mild fluorosis, the coefficient decreased from outer to middle layers, then rose toward the inner layer. Severe fluorosis enamel displayed higher friction at the outer (0.25 ± 0.044) and middle (0.18 ± 0.025) layers compared to mild fluorosis and normal enamel (p < 0.05). However, the coefficient decreased from outer to inner layers in severe fluorosis (p < 0.05) (Fig. 5).
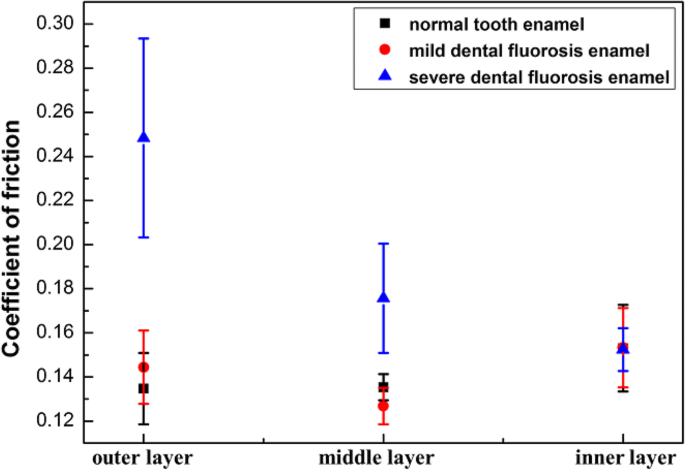
Friction coefficients of enamel layers.
Scratch depth and width increased from outer to inner layers in normal enamel (Fig. 6a). Mild fluorosis enamel showed a dip at the middle layer before rising toward the inner layer (Fig. 6b). Severe fluorosis enamel exhibited a monotonic decrease from outer to inner layers (Fig. 6c). Consequently, the outer layer of severe fluorosis enamel had the largest scratch depth and width, indicating reduced wear resistance. These observations align with prior studies linking fluoride exposure to compromised enamel wear resistance [42–46].
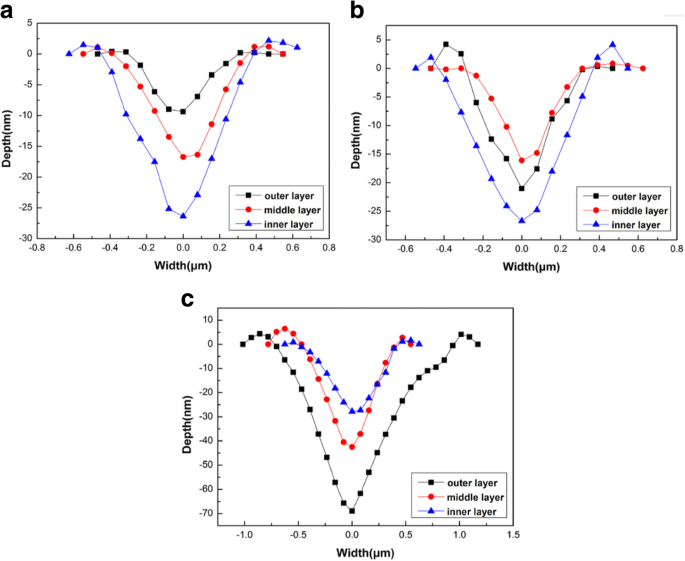
Scratch profiles of enamel layers.
Understanding these gradient properties is pivotal for selecting restorative materials that match the wear behavior of fluorosed enamel. Ceramics offer high biocompatibility and esthetics but can over‑wear opposing enamel [47, 48]. Alternatives such as PICN and composite resin blocks have been developed to provide lower wear resistance [48, 49]. PICN’s scratch metrics align with the outer layer of normal enamel, making it suitable when opposing teeth are healthy. However, when the opposing tooth is fluorosed—particularly mild fluorosis—the restorative material should mimic that enamel’s tribological profile. Lava™ ultimate (composite resin block) exhibited scratch depth and width comparable to the outer layer of mild fluorosis enamel, suggesting its suitability for fluorosed restorations. Conventional composite resin (Z350) showed higher scratch metrics, potentially leading to accelerated wear. Therefore, the mechanical compatibility of restorative materials with fluorosed enamel is essential for durable outcomes.
Nanomechanical Properties of the Normal and Abnormal Enamel Rods of Dental Fluorosis
Analysis of severe fluorosis enamel revealed two distinct rod types in the outer and middle layers: normal rods with loosely arranged crystals and abundant micropores, and abnormal rods densely packed with pores (Fig. 7). The normal rods displayed lower hardness and modulus but higher creep than abnormal rods (Fig. 8). These micro‑level variations correlate with fluorosis severity and underscore the need for restorative materials that accommodate such heterogeneity.
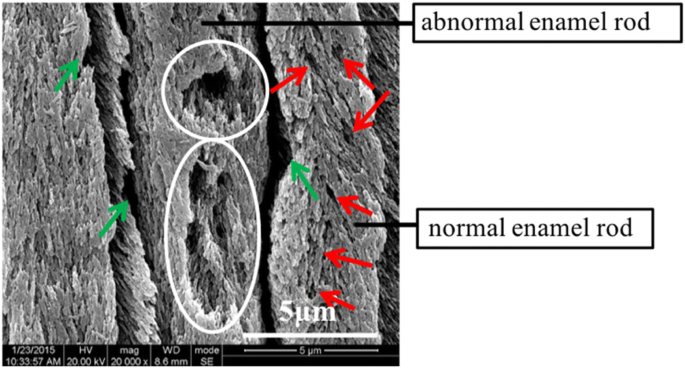
SEM image of normal and abnormal enamel rods in severe fluorosis outer layer (×20,000). Green arrows: broadened gaps; white circles: pores; red arrows: loosely arranged crystals.
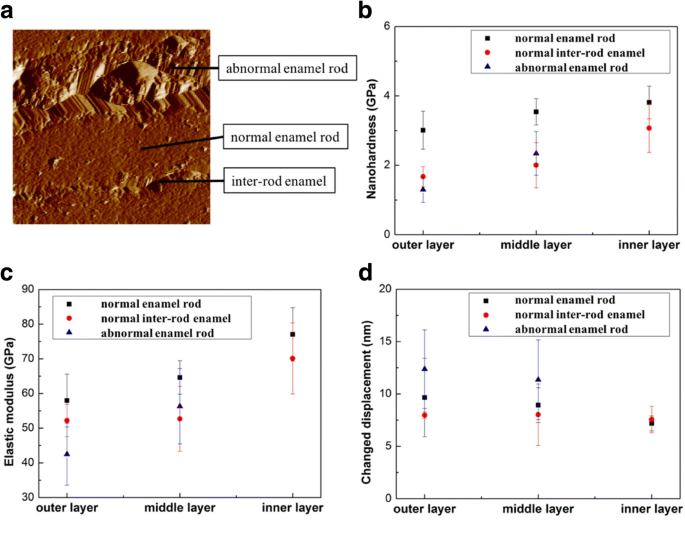
Nanomechanical properties of normal vs. abnormal rods. a Nanohardness; b Elastic modulus; c Creep behavior.
Appropriate Dental Materials for the Clinical Restoration of Dental Fluorosis
Comparative scratch analysis (Fig. 9) shows that IPS e.max CAD had the lowest scratch depth/width, PICN matched normal enamel, Lava™ ultimate aligned with mild fluorosis enamel, and Fltek™ Z350XT had the highest metrics. The outer layer of severe fluorosis enamel had the greatest scratch depth/width. These data confirm that a restorative material’s tribological profile should mirror that of the opposing fluorosed enamel to prevent accelerated wear.
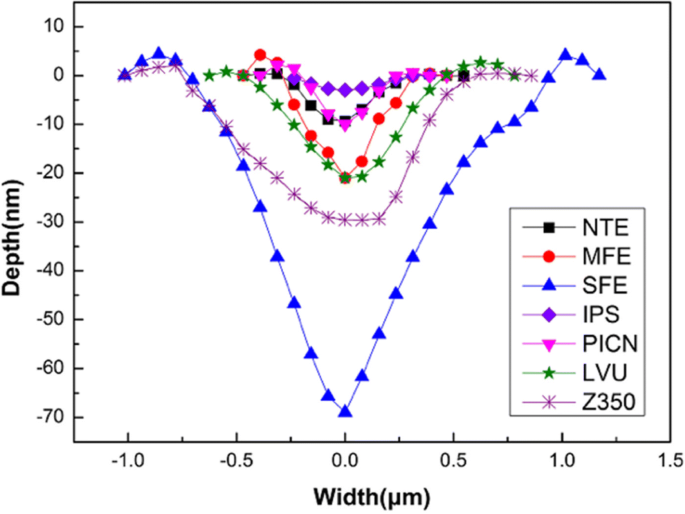
Scratch profiles on outer enamel of normal, mild, severe fluorosis and four restorative materials.
Clinical implications: fluorosis‑affected anterior teeth often require esthetic restoration, while posterior teeth may need crowns or onlays. Ceramic restorations, though esthetic, can over‑wear opposing enamel [47, 48]; PICN offers a more balanced wear profile for normal opposing enamel. For mild fluorosis, Lava™ ultimate provides a wear resistance comparable to the enamel, reducing the risk of restorative wear. In severe fluorosis, the heightened wear of the outer enamel necessitates careful material choice, potentially favoring low‑wear composites or alternative strategies.
Conclusion
Key findings:
The microstructure and gradient nanomechanical behavior of fluorosed enamel differ markedly from healthy enamel, especially in the outer layer of mild fluorosis and the outer/middle layers of severe fluorosis.
Normal and abnormal enamel rods coexist in fluorosed enamel; abnormal rods exhibit lower hardness, lower modulus, and higher creep.
Composite resin block (Lava™ ultimate) matches the wear resistance of mild fluorosis enamel and is therefore preferable to high‑wear ceramics for fluorosis restoration.
Abbreviations
- EDJ:
Enamel‑dentin junction
- IPS:
IPS e.max CAD
- LVU:
Lava™ ultimate
- MFE:
Mild dental fluorosis enamel
- NTE:
Normal tooth enamel
- PICN:
Polymer‑infiltrated‑ceramic network
- SEM:
Scanning electron microscopy
- SFE:
Severe dental fluorosis enamel
- SPM:
Scanning probe microscope
- Z350:
Fltek™ Z350XT
Nanomaterials
- The Dental Drill: History, Design, and Future of Modern Dentistry
- Reverse Engineering a Dental Clamp: 3D‑Printing a Custom Replacement Part
- Crystalline‑Si Solar Cells with a Black‑Silicon Rear Layer: Enhanced Efficiency Through Graded Band‑Gap Engineering
- Biocompatibility of Graded Nano‑Glass/Zirconia Dental Materials After Aging
- Hydrothermal Synthesis of 19 nm Sc₂O₃:Er³⁺,Yb³⁺ Nanoparticles with 4× Superior Red Upconversion Luminescence
- Energy Band Alignment in MoS₂/ZrO₂ Heterojunctions: Impact of CHF₃ Plasma Treatment
- Engineering Band Alignment in MoS₂/HfO₂ Heterojunctions via Controlled Nitridation
- Methane Adsorption on MoX₂ (S, Se, Te) Monolayers: Insights from DFT
- Hybrid PEDOT:PSS/β‑Ga2O3 Deep‑Ultraviolet Schottky Photodetectors: Temperature‑Dependent Performance Analysis
- How the Grocery Industry is Adapting to Rapid Shifts in Consumer Behavior



